Diversity, equity and inclusion (DEI) are vital components of strategic planning in a growing number of organizations across all sectors. The health care sector is especially relevant since DEI directly affects health outcomes. In the United States, most people are aware of the racial reckoning that has resulted in the necessary dialogue around implicit bias’s harmful effects. It has also drawn attention to the Black, indigenous, and people of color who are disproportionately impacted by long-standing systems that were not created with their whole personhood in mind. Together, we can foster equitable access to high-quality care for a wide range of people while building cultural competencies that increase a sense of belonging in spaces where people might not have been able to feel included before. Within neurosurgery, DEI initiatives that engage and educate teams have great potential.
One of the major goals of the Congress of Neurological Surgeons (CNS) DEI committee includes eliminating barriers to attract a diverse pool of future neurosurgical applicants. Concrete milestones with measures of success and failure support these goals, culminating in a groundbreaking program called Pathway to Neurosurgery. The CNS DEI committee developed the program to diversify applicants for neurosurgical residency. In honor of Timothy M. George, MD, FAANS, we presented the inaugural Pathway to Neurosurgery program at the CNS Annual Meeting in Austin in 2021.

2021 Pathway to Neurosurgery Program
Now led by the CNS Foundation, the program welcomes local high school students from backgrounds underrepresented in science, technology, engineering and mathematics (STEM) to the CNS Annual Meeting. A day-long symposium designed exclusively for them takes place near the general sessions so they spend the day surrounded by neurosurgeons and are introduced to considering a medical career, possibly even a career in neurosurgery. In 2021, 35 students from Austin joined us for an immersive experience at the convention center alongside other attendees of the annual meeting. Students who participated also applied for a one-year stipend and mentorship opportunity with a Dell Medical School neurosurgeon. We were thrilled to announce that two students were awarded a stipend for the year and a chance to spend one year with a local neurosurgeon. This tradition continues each year as longitudinal mentorship occurs with these students.
The Pathway to Neurosurgery program held its second event at the CNS Annual Meeting in San Francisco in 2022. On that day, 24 Oasis for Girls and San Francisco Achievers students, dressed in full surgical gowns and protective gear, visited multiple stations with tools and demonstrations used daily in neurosurgery. Volunteer neurosurgeons paired up with each student through the experiments, giving them feedback on holding surgical instruments and answering questions. Frank J. Bova, MD, PhD, kept a crowd of students’ interest as he described how to place an external ventricular drain shipped to San Francisco from the University of Florida just for the occasion.

2023 Pathway to Neurosurgery Program
“This is how I practice!” said an early career neurosurgeon to a wide-eyed high schooler, trying not to grip the egg too tightly as she carefully drilled through the shell. “Everyone has become involved in making this a great event for the kids,” said Maryam Rahman, MD, FAANS, one of the spearheads of the original program. Between station rotations, the students listened to speakers from various backgrounds talk about their own pathways to becoming neurosurgeons.
“I am passionate about the Pathway to Neurosurgery program because I know how meaningful it is to see someone like me in a STEM field. I spent my young life repeatedly told that I would never be a neurosurgeon. Neurosurgery must be a career option for them because we need more neurosurgeons that represent our broad spectrum of patients”, states Tiffany R. Hodges, MD, chair of the CNS Foundation’s DEI Committee.
During lunch, volunteer neurosurgeons sat at round tables with the students and casually answered their questions. Laughter and conversation bubbled throughout the day. Not only were the students enjoying themselves, but volunteer neurosurgeons also said it was one of the highlights of the CNS Annual meeting.

2023 Pathway to Neurosurgery Program
Weeks later, the CNS Foundation received feedback from many of the guests. “I never even heard of neurosurgery before I came to the event,” replied one student. “Now I’m seriously considering it for my future.” Mission accomplished.
The CNS Foundation hosted its third annual Pathway to Neurosurgery Program in Washington, D.C., during the CNS Annual Meeting in September 2023. It was a very successful event, and in recognition of this noteworthy program, the District of Columbia Mayor Muriel Bower proclaimed Sept. 7-13 as Pathway to Neurosurgery Week.
The CNS Foundation is excited to continue to expand this program.
Editor’s Note: We hope you will share what you learn from our posts in the Making and Maintaining a Neurosurgeon series. We invite you to join the conversation on Twitter by following @Neurosurgery and using the hashtag #Neurosurgery.

Tiffany R. Hodges, MD
Co-Chair, CNS DEI Committee
University Hospitals
Cleveland, Ohio



 Aladine A. Elsamadicy, MD
Aladine A. Elsamadicy, MD
 Lola B. Chambless, MD, FAANS
Lola B. Chambless, MD, FAANS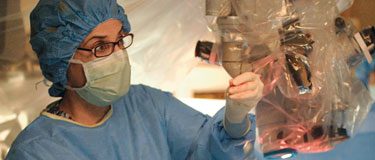



 Krystal L. Tomei, MD, MPH, FAANS, FACS, FAAP
Krystal L. Tomei, MD, MPH, FAANS, FACS, FAAP David A. Paul, MD, MS
David A. Paul, MD, MS




 The Department of Neurosurgery at Stanford University is committed to inclusive excellence at all levels of education and training. Investing in outreach and pipeline programs exposes students to knowledge and opportunities otherwise unavailable. Our reach extends beyond Stanford and the surrounding community — we have reached students from all over the world who are interested in the neurosciences and are dedicated to learning. We are proud of the department’s work with outreach, including students locally, nationally and internationally. The future of neuroscience is bright.
The Department of Neurosurgery at Stanford University is committed to inclusive excellence at all levels of education and training. Investing in outreach and pipeline programs exposes students to knowledge and opportunities otherwise unavailable. Our reach extends beyond Stanford and the surrounding community — we have reached students from all over the world who are interested in the neurosciences and are dedicated to learning. We are proud of the department’s work with outreach, including students locally, nationally and internationally. The future of neuroscience is bright.

 Julia Blanchet
Julia Blanchet Maria Ceja
Maria Ceja
 Reena P. Thomas, MD, PhD
Reena P. Thomas, MD, PhD Krystal L. Tomei, MD, MPH, FAANS, FACS, FAAP
Krystal L. Tomei, MD, MPH, FAANS, FACS, FAAP