 Guest post from Kim Pollock, RN, MBA, CPC, CMDP (left) and Teri Romano, RN, MBA, CPC, CMDP (right)
Guest post from Kim Pollock, RN, MBA, CPC, CMDP (left) and Teri Romano, RN, MBA, CPC, CMDP (right)
KarenZupko & Associates, Inc.
The Centers for Medicare & Medicaid Services (CMS) is requiring all HIPAA-covered entities (e.g., physicians, facilities, health insurers) to use ICD-10 codes for services performed on Oct. 1, 2015 or later. Are you ready? A recent survey by Karen Zupko & Associates, Inc., showed that more than one-quarter of the 647 practices responding had not started preparing for this biggest change in healthcare coding since ICD-9 was implemented in 1979. The countdown to the Oct. 1 compliance date is 51 days, so if you haven’t already done so, the time to start getting ready for this coding system conversion is now!
Here are our top tips for ensuring a smooth transition to ICD-10:
1. Inventory your practice to determine:
- What documents need updating, such as practice encounter forms/superbills and the surgery scheduler cheat sheets;
- Who will need neurosurgery-specific ICD-10 education and training (e.g., neurosurgeons, residents, fellows, non-physician practitioners, billers, coders); and
- How you will provide this education and training (e.g., AANS course, on-site education) and when it will occur – hopefully before Oct. 1, 2015!
2. Run an ICD-9 frequency report, from your practice management information system, for each provider to determine the most frequently used diagnosis codes; there are usually 20-30 more commonly used codes. You will do this for each provider to determine differences for subspecialties (e.g., spine, cerebrovascular).
3. Map the most frequently used diagnosis codes from ICD-9 to ICD-10. Be sure to map to the ICD-10 code(s) with the highest level of specificity and avoid mapping to “unspecified” codes. The point of using ICD-10 is for a higher level of specificity than what ICD-9 allows.
Some codes will have a one to many code mapping ratio, such as carpal tunnel syndrome shown in the example below.
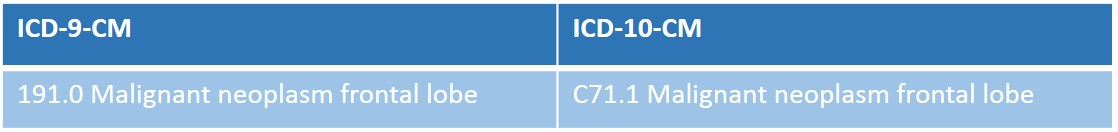
Other codes will have a 1:1 ratio such as the tumor diagnosis codes as shown below.
4. Review current provider documentation to determine if it is “code-able” in ICD-10. If so, great! If not, discuss the missing information with the provider to ensure future documentation has all necessary information to assign the correct ICD-10 code.
5. Dual code until Oct. 1, 2015. Code using ICD-10 at least one service per provider every day to become familiar with the codes and necessary documentation. Practice makes perfect!
6. Eliminate paper and use your EHRs electronic charge capture tool for office services. Save trees by not using a paper superbill (aka encounter form, charge ticket). Mapping to ICD-10 all the diagnosis codes on your current paper charge ticket will make the new one several pages long which is not a sustainable option.
7. Sharpen practice collection skills. All sources are predicting cash flow slowdowns with ICD-10 implementation. If you are collecting at 85 percent functionality, that’s not good enough – work now to improve.
8. Be financially prepared for cash flow issues on Oct. 1, 2015. Do not empty the bank account with end of 3rd quarter doctor bonuses. Reserve money “just in case.” Obtain a line of credit (LOC) now from your bank in case you need it in October if you are not willing to go without a salary for a few weeks or months while the predicted payment delays occur. Banks are not likely to lend you money when you need it; or they will charge you a higher interest rate at that point. Obtain a LOC now when you don’t need it.
While CMS recently announced flexibility guidance that allows for additional flexibility in the claims auditing and quality reporting processes related to ICD-10, ongoing preparations starting now for ICD-10 implementation will help your practice smoothly transition to the new diagnosis coding set on Oct. 1, 2015.






Great post! Thanks for sharing your best techniques on neurosurgery with us,it is very useful to me.